
Menopause is a natural biological process that marks the end of a woman’s reproductive years. It is a time of significant hormonal changes, with the body gradually producing less estrogen and progesterone. While menopause affects women in various ways, one common impact is its effect on resilience to stress.
Resilience refers to an individual’s ability to adapt and bounce back in the face of challenging situations. It is an important aspect of mental and emotional well-being, helping individuals navigate the ups and downs of life. However, during menopause, the hormonal fluctuations can disrupt this resilience, making women more susceptible to stressors.
Stress is a normal part of life, but during menopause, the combination of hormonal changes and external stressors can create a perfect storm. The decrease in estrogen can affect the brain’s stress response system, leading to increased sensitivity and reactivity to stress. This can manifest in symptoms such as irritability, anxiety, and mood swings, further exacerbating the impact of stress on overall well-being.
Understanding the impact of menopause on resilience to stress is crucial for women going through this transitional phase. By recognizing the physiological changes happening in their bodies, women can better equip themselves to manage stress and build resilience. This may involve seeking support from healthcare professionals, adopting stress management techniques such as mindfulness and exercise, and making lifestyle adjustments to prioritize self-care.
The Effects of Menopause on Stress Resilience
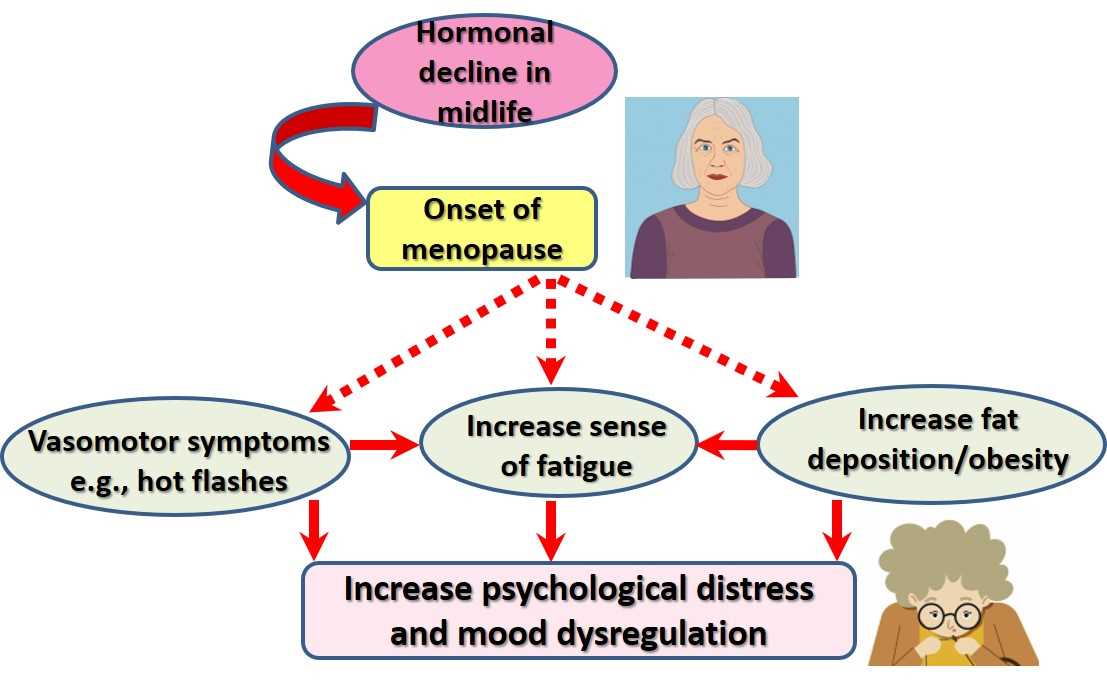
Menopause is a natural process that occurs in women usually in their late 40s or early 50s, marking the end of their reproductive years. It is characterized by a decrease in the production of estrogen and other hormones, leading to various physical and psychological changes.
One significant impact of menopause is its effect on stress resilience. Resilience refers to an individual’s ability to cope with and bounce back from stressful situations. It is an important factor in maintaining overall mental health and well-being.
Studies have shown that menopause can lower resilience to stress, making women more susceptible to its negative effects. The hormonal changes during menopause can disrupt the delicate balance of neurotransmitters in the brain that regulate mood and stress response.
Estrogen, in particular, plays a crucial role in modulating the stress response. It helps regulate the release of stress hormones like cortisol and influences the functioning of neurotransmitters such as serotonin and dopamine. During menopause, the decline in estrogen levels can lead to dysregulation of these systems, making women more vulnerable to the impact of stress.
In addition to hormonal changes, menopause also brings about other physical and psychological symptoms that can contribute to decreased stress resilience. Hot flashes, night sweats, sleep disturbances, and mood swings are common symptoms experienced by women during this transitional phase. These symptoms can disrupt sleep patterns, increase fatigue, and affect overall emotional well-being, making it harder for women to cope with stressors.
Furthermore, the psychological impact of menopause, such as changes in body image, self-esteem, and sexual function, can also contribute to decreased resilience to stress. The combination of physical and psychological changes can create a perfect storm for increased vulnerability to stress and its negative consequences.
It is important for women going through menopause to prioritize self-care and seek support from healthcare professionals. Regular exercise, healthy eating, stress management techniques, and social support can all help improve stress resilience during this transitional phase. Additionally, hormone replacement therapy may be considered in some cases to alleviate symptoms and support overall well-being.
| Key Points: |
|---|
| – Menopause can lower resilience to stress. |
| – Hormonal changes during menopause can disrupt the balance of neurotransmitters that regulate mood and stress response. |
| – Physical and psychological symptoms of menopause can contribute to decreased stress resilience. |
| – Self-care, support, and hormone replacement therapy can help improve stress resilience during menopause. |
Hormonal Changes and Stress Response
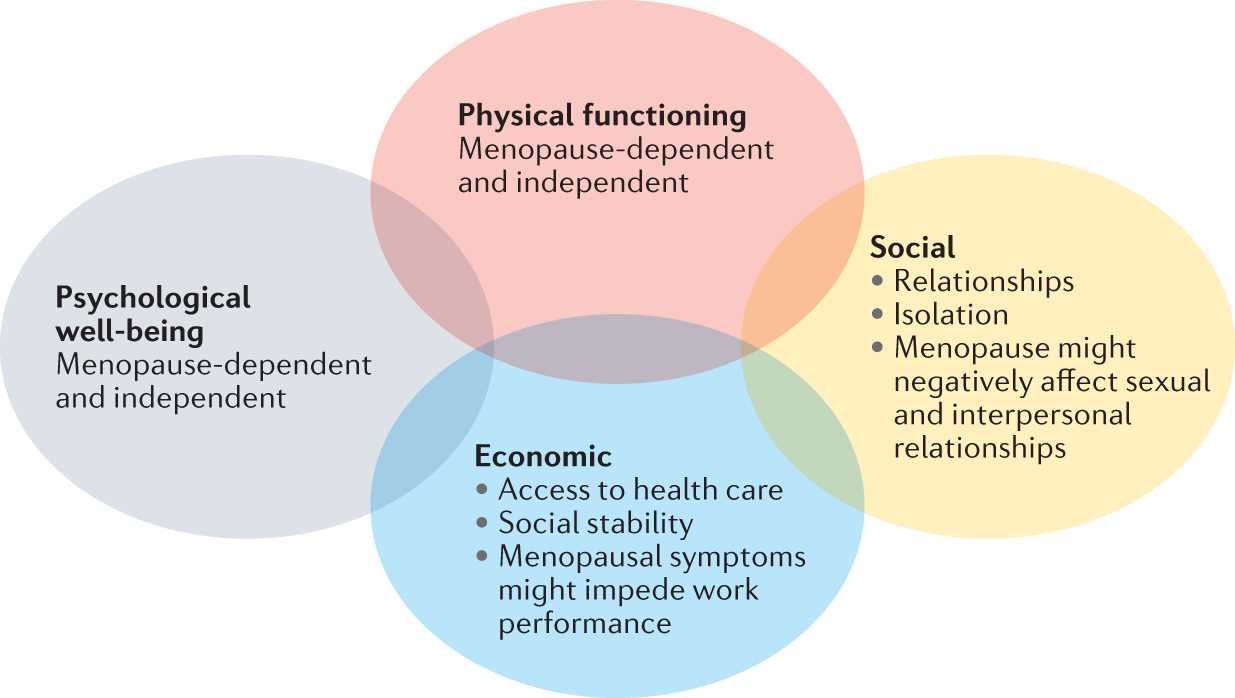
During menopause, women experience significant hormonal changes that can impact their stress response. The decline in estrogen levels during menopause is believed to contribute to a lower resilience to stress.
Estrogen plays a crucial role in regulating the stress response in the body. It helps to maintain the balance of cortisol, a hormone released in response to stress. When estrogen levels decrease, cortisol levels can become dysregulated, leading to an exaggerated stress response.
This hormonal imbalance can result in a variety of symptoms, including increased anxiety, irritability, and difficulty coping with stress. Women may find themselves feeling overwhelmed by situations that they previously handled with ease.
Additionally, the hormonal changes during menopause can also impact the functioning of the hypothalamic-pituitary-adrenal (HPA) axis, which is responsible for regulating the body’s response to stress. This can further contribute to a lower resilience to stress.
It is important for women going through menopause to be aware of these hormonal changes and their impact on stress. Seeking support from healthcare professionals and implementing stress management techniques can help improve resilience and overall well-being during this transition.
| Key Points: |
|---|
| – Menopause leads to hormonal changes that can affect the stress response. |
| – Decreased estrogen levels can result in dysregulated cortisol levels. |
| – Hormonal changes can impact the functioning of the HPA axis. |
| – Seeking support and implementing stress management techniques can help improve resilience during menopause. |
Impact on Emotional Well-being

The menopause can have a significant impact on a woman’s emotional well-being, particularly in relation to her resilience to stress. As women go through menopause, the hormonal changes that occur can lead to increased feelings of anxiety, irritability, and mood swings.
Resilience, which is the ability to adapt and cope with stress, can be affected by the hormonal fluctuations that come with menopause. Estrogen, a hormone that plays a key role in regulating mood, decreases during menopause. This decrease in estrogen can lead to a decrease in resilience, making women more susceptible to the negative effects of stress.
Stress can have a profound impact on emotional well-being. It can exacerbate feelings of anxiety and irritability, and can also contribute to the development or worsening of mood disorders such as depression. For women going through menopause, the combination of hormonal changes and increased stress can create a perfect storm for emotional distress.
It is important for women going through menopause to prioritize their emotional well-being and seek support if needed. This may involve talking to a healthcare professional or therapist who can provide guidance and help develop coping strategies. Additionally, engaging in stress-reducing activities such as exercise, mindfulness, and relaxation techniques can also be beneficial in managing the emotional impact of menopause.
| Impact | Emotional Well-being |
|---|---|
| Resilience to stress | Decreased |
| Mood swings | Increased |
| Anxiety | Increased |
| Irritability | Increased |
Cognitive Effects

Menopause is known to lower resilience to stress, and one of the areas where this impact is most evident is in cognitive function. Many women going through menopause experience difficulties with memory, concentration, and overall cognitive performance. This can be attributed to the hormonal changes that occur during menopause, specifically the decrease in estrogen levels.
Estrogen plays a crucial role in maintaining cognitive function, and its decline during menopause can have a significant impact on the brain. Studies have shown that women going through menopause may experience changes in brain structure and function, including reduced volume in certain regions and alterations in neural networks.
These cognitive effects can manifest in various ways. Some women may notice that they have trouble remembering things or have difficulty staying focused on tasks. Others may experience mental fog or have trouble processing information quickly. These symptoms can be frustrating and impact daily life and work performance.
It is important for women going through menopause to be aware of these cognitive effects and seek support if needed. There are strategies and interventions that can help mitigate the impact of menopause on cognitive function. These may include lifestyle changes, such as exercise and a healthy diet, as well as cognitive training exercises and hormone therapy.
By understanding the cognitive effects of menopause, women can better navigate this stage of life and proactively address any challenges that arise. With the right support and interventions, it is possible to maintain cognitive function and overall well-being during menopause.
Biological Mechanisms Behind the Decreased Resilience
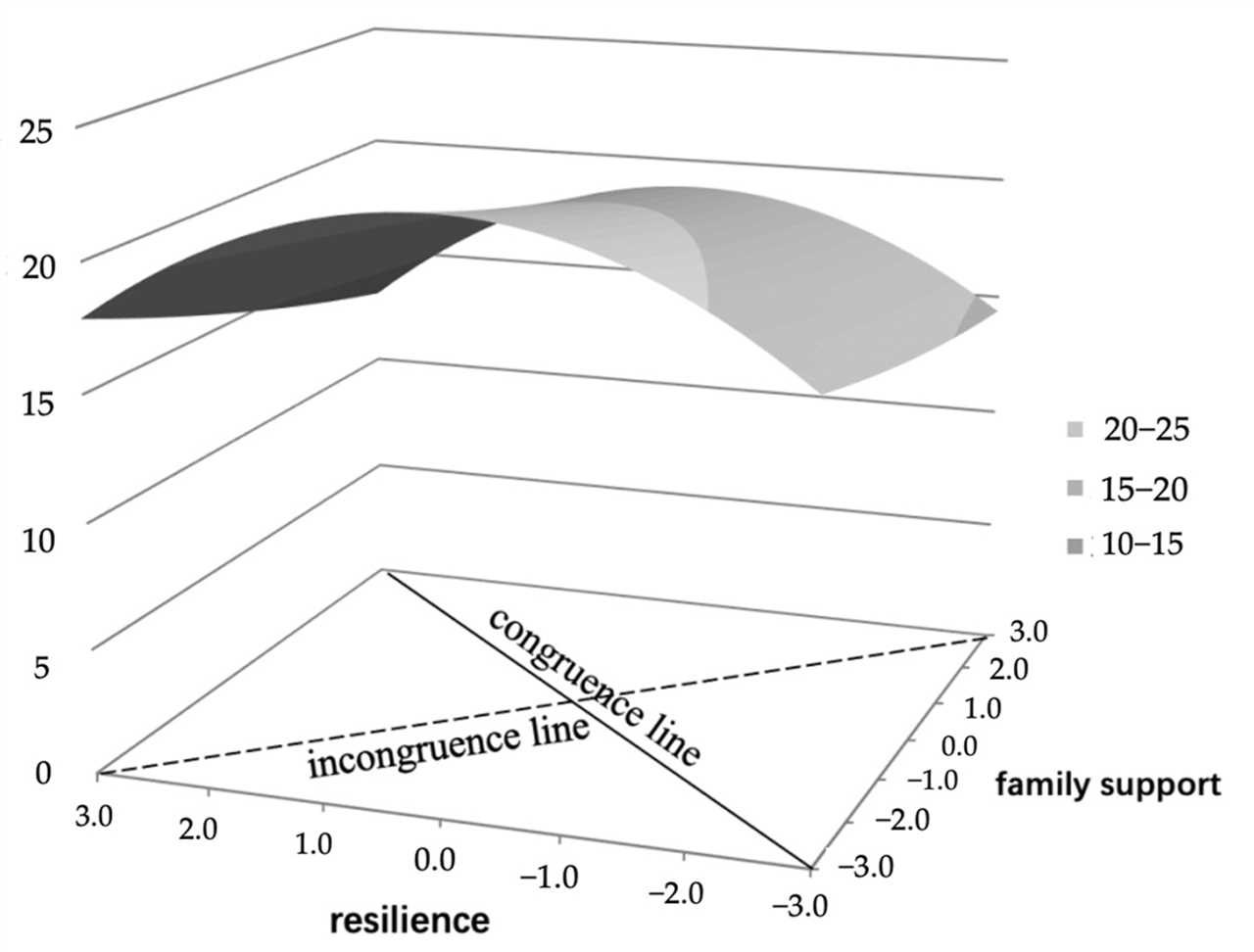
Menopause is a natural process that occurs in women as they age, marking the end of their reproductive years. During this time, hormonal changes take place in the body, leading to a variety of physical and psychological symptoms. One of the effects of menopause is a decrease in resilience to stress.
Resilience refers to the ability to adapt and cope with stressors, maintaining psychological and physical well-being. It is an essential trait that helps individuals navigate through life’s challenges. However, during menopause, the biological mechanisms that support resilience are disrupted.
One of the key factors contributing to the decreased resilience during menopause is the decline in estrogen levels. Estrogen is a hormone that plays a crucial role in regulating the body’s response to stress. It has been shown to have a protective effect on the brain, promoting neuroplasticity and enhancing the functioning of the stress response system.
Additionally, estrogen has been found to modulate the production and regulation of neurotransmitters such as serotonin and dopamine. These neurotransmitters play a vital role in mood regulation and emotional well-being. The decline in estrogen levels during menopause can lead to imbalances in these neurotransmitters, contributing to increased vulnerability to stress.
Furthermore, estrogen has anti-inflammatory properties and helps regulate the immune system. It has been observed that menopausal women have higher levels of inflammation markers, indicating increased inflammation in the body. Chronic inflammation has been linked to various health problems, including increased susceptibility to stress-related disorders.
Another biological mechanism underlying the decreased resilience to stress during menopause is the impact on the hypothalamic-pituitary-adrenal (HPA) axis. The HPA axis is responsible for regulating the body’s stress response, including the release of cortisol, a hormone involved in the stress response. During menopause, the dysregulation of the HPA axis can lead to an overactive stress response system, making women more susceptible to the negative effects of stress.
In conclusion, the biological mechanisms behind the decreased resilience to stress during menopause are multifaceted. The decline in estrogen levels, imbalances in neurotransmitters, increased inflammation, and dysregulation of the HPA axis all contribute to this phenomenon. Understanding these mechanisms can help develop targeted interventions and support systems to enhance resilience and well-being during this transitional phase of a woman’s life.
Estrogen and Its Role in Stress Regulation
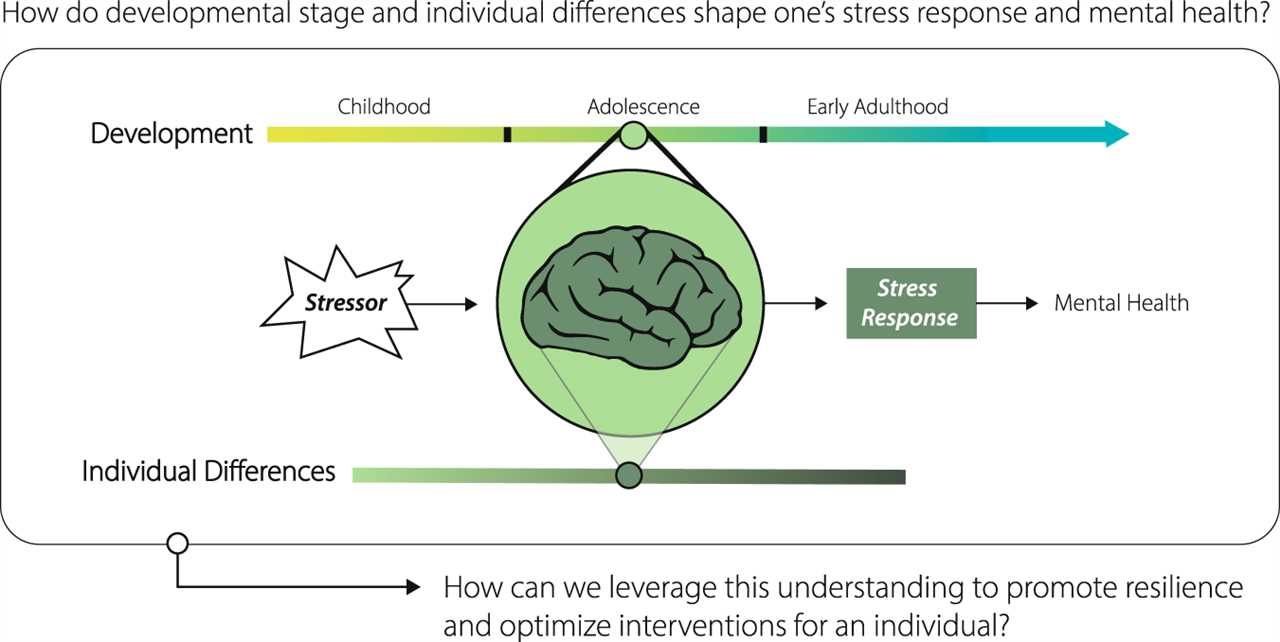
Estrogen, a hormone that plays a crucial role in the reproductive system, also has a significant impact on stress regulation. During menopause, when estrogen levels decline, women may experience a decrease in resilience to stress.
Estrogen has been found to regulate the production and release of stress hormones, such as cortisol, in the body. It helps to maintain the balance between the sympathetic and parasympathetic nervous systems, which are responsible for the body’s stress response.
When estrogen levels are low, the body’s stress response may become dysregulated, leading to an increased sensitivity to stressors. This can result in a heightened emotional response, difficulty in coping with stress, and a reduced ability to bounce back from stressful situations.
Furthermore, estrogen has been found to have neuroprotective effects on the brain. It helps to maintain the health and function of brain cells, particularly in regions involved in stress regulation, such as the amygdala and hippocampus.
Studies have shown that estrogen can enhance the resilience to stress by reducing the activation of the amygdala, which is responsible for the fear and anxiety response. It also promotes the growth and survival of neurons in the hippocampus, which is involved in memory and emotional regulation.
Overall, estrogen plays a crucial role in stress regulation, and its decline during menopause can contribute to a decrease in resilience to stress. Understanding the impact of estrogen on stress can help in developing strategies to manage stress more effectively during this transitional phase of life.
Neurotransmitter Imbalance and Mood Disorders

Menopause, a natural process that marks the end of a woman’s reproductive years, can have a significant impact on her physical and mental health. One of the key changes that occur during menopause is a decline in the production of certain hormones, including estrogen and progesterone.
These hormonal changes can disrupt the delicate balance of neurotransmitters in the brain, leading to an imbalance that can contribute to mood disorders such as depression and anxiety. Neurotransmitters are chemical messengers that help regulate various functions in the brain, including mood, sleep, and appetite.
Estrogen plays a crucial role in maintaining the balance of neurotransmitters, particularly serotonin, dopamine, and norepinephrine. Serotonin is often referred to as the “feel-good” neurotransmitter, as it helps regulate mood and promotes feelings of well-being. Dopamine is involved in motivation and reward, while norepinephrine helps regulate the body’s response to stress.
During menopause, the decline in estrogen levels can lead to a decrease in the production of these neurotransmitters. This imbalance can result in symptoms such as mood swings, irritability, and difficulty coping with stress.
Stress can further exacerbate the neurotransmitter imbalance during menopause. The body’s stress response system, known as the hypothalamic-pituitary-adrenal (HPA) axis, becomes dysregulated during this time. This dysregulation can lead to increased production of stress hormones, such as cortisol, which can further disrupt the balance of neurotransmitters.
Understanding the connection between menopause, neurotransmitter imbalance, and mood disorders is crucial for developing effective strategies to support women during this transitional period. Hormone replacement therapy (HRT) and lifestyle changes, such as regular exercise and stress reduction techniques, can help restore the balance of neurotransmitters and improve resilience to stress.
- Menopause can disrupt the balance of neurotransmitters in the brain.
- Estrogen plays a crucial role in maintaining the balance of neurotransmitters, including serotonin, dopamine, and norepinephrine.
- The decline in estrogen levels during menopause can lead to a decrease in the production of these neurotransmitters, resulting in mood disorders.
- Stress can further exacerbate the neurotransmitter imbalance during menopause.
- Understanding this connection is crucial for developing effective strategies to support women during this transitional period.
Inflammation and Stress Response

Menopause is a natural process that occurs in women as they age, and it is characterized by the cessation of menstrual periods. This hormonal change can have a significant impact on a woman’s overall health and well-being. One area that is particularly affected is the body’s response to stress.
During menopause, the levels of estrogen and progesterone in a woman’s body decrease. These hormones play a crucial role in regulating the body’s inflammatory response and stress levels. As a result, the body becomes more susceptible to inflammation and has a lower resilience to stress.
Inflammation is a natural response of the immune system to protect the body from injury or infection. However, when inflammation becomes chronic, it can lead to a range of health problems, including cardiovascular disease, diabetes, and autoimmune disorders. The decrease in estrogen and progesterone during menopause can contribute to increased inflammation in the body.
Additionally, the hormonal changes during menopause can also affect the body’s stress response. The stress response is a complex physiological reaction that helps the body cope with challenging situations. However, when the body is unable to effectively manage stress, it can lead to chronic stress, which can have detrimental effects on health.
Research has shown that the lower levels of estrogen and progesterone during menopause can disrupt the body’s stress response system. This disruption can lead to increased levels of stress hormones, such as cortisol, and a decreased ability to cope with stress. As a result, menopausal women may experience heightened stress levels and a reduced ability to handle stressful situations.
In conclusion, the hormonal changes that occur during menopause can have a significant impact on the body’s inflammatory response and stress levels. The decrease in estrogen and progesterone can lead to increased inflammation and a lower resilience to stress. It is important for menopausal women to be aware of these changes and take steps to manage their stress levels and promote overall well-being.
Lifestyle Factors Affecting Resilience During Menopause

During menopause, several lifestyle factors can significantly lower a woman’s resilience to stress. Stress is a natural response to challenging situations, but it can have a negative impact on overall well-being if not managed effectively. Menopause brings about hormonal changes that can make women more susceptible to stress, and certain lifestyle choices can exacerbate this effect.
One lifestyle factor that can lower resilience to stress during menopause is a sedentary lifestyle. Lack of physical activity not only affects physical health but also mental well-being. Regular exercise has been shown to reduce stress levels and improve resilience. Engaging in activities such as walking, swimming, or yoga can help manage stress and improve overall resilience during menopause.
Another lifestyle factor that can impact resilience during menopause is poor sleep quality. Hormonal fluctuations during menopause can disrupt sleep patterns, leading to insomnia or poor sleep quality. Lack of adequate sleep can increase stress levels and make it more difficult to cope with daily challenges. Establishing a regular sleep routine, creating a relaxing bedtime environment, and avoiding stimulants such as caffeine can help improve sleep quality and enhance resilience during menopause.
Nutrition is another crucial lifestyle factor that can influence resilience during menopause. A diet high in processed foods, sugar, and unhealthy fats can negatively affect both physical and mental health. These types of foods can contribute to inflammation in the body, which can increase stress levels. On the other hand, a diet rich in fruits, vegetables, whole grains, and lean proteins can provide essential nutrients and antioxidants that support resilience and overall well-being during menopause.
Lastly, social support plays a vital role in resilience during menopause. Having a strong support system, whether it be friends, family, or a support group, can help women navigate the challenges of menopause and reduce stress levels. Connecting with others, sharing experiences, and seeking emotional support can contribute to increased resilience and a better overall well-being during this transitional phase.
In conclusion, several lifestyle factors can impact resilience during menopause. Adopting a physically active lifestyle, prioritizing sleep quality, maintaining a healthy diet, and seeking social support are essential for managing stress and enhancing resilience during this phase of life.
Physical Activity and Stress Reduction
Physical activity has long been known to have numerous benefits for overall health and well-being. One of the key benefits of regular physical activity is its ability to reduce stress and improve resilience to stressors. This is particularly important for individuals experiencing menopause, as they may have lower resilience to stress due to hormonal changes.
Engaging in regular physical activity can help to lower stress levels by releasing endorphins, which are natural mood-boosting chemicals in the brain. These endorphins can help to improve mood and reduce feelings of anxiety and depression. Additionally, physical activity can provide a distraction from stressors and help individuals to focus on the present moment.
Furthermore, physical activity can also improve resilience to stress by improving overall physical health. Regular exercise can help to strengthen the cardiovascular system, increase lung capacity, and improve muscle tone. This can result in increased energy levels and improved ability to cope with stressors.
There are many different types of physical activity that can be effective in reducing stress. These can include aerobic exercises such as walking, running, or cycling, as well as strength training exercises and mind-body practices such as yoga or tai chi. It is important to find activities that are enjoyable and sustainable in order to maintain a regular exercise routine.
In conclusion, physical activity can play a crucial role in reducing stress and improving resilience to stressors, particularly for individuals experiencing menopause. Incorporating regular exercise into daily routines can help to release endorphins, improve overall physical health, and provide a distraction from stressors. By prioritizing physical activity, individuals can enhance their resilience and better cope with the challenges of menopause.
Nutrition and Hormonal Balance

Nutrition plays a crucial role in maintaining hormonal balance during menopause. The hormonal changes that occur during this phase can have a significant impact on a woman’s resilience to stress. A well-balanced diet can help alleviate some of the symptoms associated with menopause and improve overall well-being.
During menopause, the body undergoes a decline in estrogen production, which can lead to a variety of physical and emotional symptoms. These symptoms, such as hot flashes, mood swings, and fatigue, can increase stress levels and make it more difficult to cope with daily challenges.
Ensuring adequate nutrition is essential for supporting hormonal balance during menopause. Certain nutrients, such as phytoestrogens found in soy products, can help mimic the effects of estrogen in the body and alleviate some of the symptoms associated with hormonal fluctuations.
In addition to phytoestrogens, other nutrients that are important for hormonal balance include omega-3 fatty acids, vitamin D, and magnesium. Omega-3 fatty acids, found in fatty fish like salmon and flaxseeds, can help reduce inflammation and support brain health, which can be beneficial for managing stress and improving resilience.
Vitamin D is crucial for maintaining bone health and supporting the immune system. It has also been linked to mood regulation and may help alleviate symptoms of depression and anxiety, which can be exacerbated during menopause.
Magnesium is another essential nutrient that plays a role in hormonal balance. It helps regulate neurotransmitters in the brain, which can influence mood and stress levels. Good sources of magnesium include leafy green vegetables, nuts, and whole grains.
It’s important to note that every woman’s nutritional needs during menopause may vary, and it’s best to consult with a healthcare professional or registered dietitian to develop a personalized nutrition plan. By incorporating a well-balanced diet that includes these essential nutrients, women can support hormonal balance and improve resilience to stress during menopause.

I am Patrina de Silva, a psychologist and mental health blogger in Sri Lanka. After obtaining psychology degrees from the University of Colombo and Monash University, I returned home to work as a counselor while also starting the popular blog “Pressy but Happy” to provide advice on psychological issues. Over the past decade, my empathetic articles have made my blog a leading mental health resource in the country. In addition to writing, I maintain a private therapy practice, frequently volunteer counseling time, and conduct seminars, driven by my passion for destigmatizing mental illness and educating the public on the mind-body connection. I strive to be an influential voice in my field through my compassionate approach.
